{ Read Birth Story Part 1: Delivery here. }
After DH left the OR, he called my dad to let him know the baby was born and that things weren’t going so well for me. He texted my brother, Teddy, in London. As it happened, Teddy was with our mum, step-dad, and sister. And then he called my BFF, Boo, to let her know what was going on. Boo said she knew something was wrong before he called. She was in a meeting and had her phone out, awaiting news of V’s birth to arrive around 9:15am. I think DH called her around an hour later than expected. It was strange to be told what people were doing. You might think that, lying on the operating table, I would be daydreaming about DH calling my loved ones, but it never occurred to me. I was very much focused on what was happening to my body. I was calm, but frightened in a helpless way, trusting that Dr. D could fix the problem. She didn’t let me down.
First Hours
After I left the OR, I was wheeled back to the space I’d occupied before surgery and OR nurse Gena got me settled. Dr. D stopped by soon after and although she didn’t go into much detail at that point, she let me know that it was a serious caesarean, and that DH and V were in the NICU. “V is okay, but her breathing was a little fast, so they wanted to keep an eye on her.” She explained that had things gone smoothly for me they would have done this in the OR, but they needed the space. Dr. D’s visit was short, and she said she was going to get DH and the baby.
As I waited for my husband and daughter to appear, I concentrated on trying to wiggle my toes. I was able to slightly raise my knees and move my left big toe. So this is what it must be like to be paralysed. I was brimming with anticipation when Gena cried, “Here they are!” and I saw DH rounding the curtain with a small bundle in his arms.
I don’t have as clear a memory as I would like of the moment V was placed into my arms. I was still a bit spacey from the Duramorph so the rest of the day is hazy. At the time I felt compos mentis, but it’s hard to recall what happened and when. A few moments, helped by texts and photos, stand out.
I remember the joyful relief of taking her into my arms. I remember holding her and whispering Hi! Hi! but not really how I felt. I think this amnesia was caused partly the morphine I took that night, as well as trauma amnesia. But I do remember feeling distantly euphoric, and, true to my troubleshooting nature, immediately wanting to take steps to breastfeed – V was already more than two hours old by the time she was placed into my arms. I unwrapped her from her swaddle and held her against my bare chest. I reminded Gena that I wanted to see a lactation consultant ASAP.
In recovery, I began to learn just how serious things had been in the OR. Gena told me that if I had delivered in a “more rural setting” I could have died. She said I lost 3,600 ml of blood – a few ounces shy of a gallon. The average human body has about 5 litres / 1.5 gallons, so I lost about ⅔ of all the blood in my body. (Of course, much of what I lost was transfused blood, but it’s still sobering…) She said she was amazed by how well I was doing, that what I had been through “on paper” didn’t match the woman sitting up and smiling before her. I was triumphant. Fuck the birth plan – V is healthy and I have my uterus. I delivered this baby against the odds and I survived!
I watched as DH changed his first ever diaper. I suggested he put V between my outstretched legs and watched as Gena assisted him. Wipe front to back, I reminded him. Seeing as how I couldn’t change my daughter’s diaper myself, I asked him to take a picture of her little butt covered in meconium. It would be several days before I changed a diaper, so I’m glad I have pictures of her first poop.
I remembered that my parents-in-law were in the waiting room and suggested they be brought back to recovery. I knew they had already met V, but I wanted to show her off again. Knowing my MIL, she would be sick with worry and I was right. I saw the look of relief on their faces when they saw I was okay, and joy when they saw V.
After seeing DH’s parents delight in meeting their newest granddaughter, I thought of my own. I asked for my phone so I could group text my family and let them know I was okay. Coincidentally, at that very moment, my brother texted me via WhatsApp.
Teddy: Hope everything’s okay. We’re all with you! Keep us posted x
Me: I’m okay!
Bubs: Horray!
Teddy: Is that you lauren?
Me: Yes, Lauren
Teddy: How are you??
Pa: Hooray! So relieved. Love you so much. Congratulations Mum!
Teddy: Ma speaking. Oh thank god. I was so worried. Brave girl. I love you so much. Xxx
My family’s palpable concern and relief was like biofeedback: things really had been serious in the OR and it genuinely hadn’t occurred to me before then that DH would have done the right thing to let them know what was going on and that they would be rightly concerned.
The phone reception wasn’t great, and although the photo I tried to send didn’t go through, pictures from everyone started coming through. My mum, step-dad, brother, and sister having dinner in London and raising their glasses of white wine; my dad and his girlfriend in Bulgaria clinking after dinner glasses of red wine; my step-sister and her husband in Ecuador toasting us with gins and tonic, and their young daughter stuffing her red butterfly-painted face.
After a caesarean, you stay in recovery until your spinal block has worn off. When you can move your legs again, you’re transferred to the Family and Maternity Care Center (FMCC). I ended up spending the night on the delivery ward because I needed one-on-one care.
As the afternoon wore on, my spinal block and OR chill pills wore off. The more time that passed, the less like myself I became: the smiling woman Gena witnessed sitting up in bed began to fade and was replaced by someone I’d never been before. I couldn’t raise my hips for her to give me a sanitary pad and cried out with the pain. Gena was awesome. Instead of forcing me, she slid an absorbent square pad under my bottom and pulled it up between my legs. When asked how much pain I was in on a scale from 0-10, I said 9 – because surely a 10 would be reserved for an amputation – but I was in so much pain I could barely breathe. I couldn’t cry out or even grit my teeth because they chattered with the adrenaline of being in so much pain. I felt like I’d been hit by a truck, and in a sense I had been. Having someone’s hands, no matter how skilled, rummaging around in your abdomen for almost three hours fucking hurts afterwards.
I was desperate to stay on top of my pain, mainly because I wanted to breastfeed and pain will inhibit milk production. But now that the pain was here I couldn’t think about anything other than making it go away. I was plied with medication, but nothing worked — at best the pain dropped to a 5 or 6. I have a high pain threshold, so it was quite shocking to me to experience so much pain. Gena paged Dr. A, the anaesthesiologist. Together with DH they agreed that I would be given self-administered morphine. I’d get 2mg every 20 minutes, just by pressing a button. It sounded like a fantastic plan to me, but it takes a while to get set up – I’m guessing because Patient-Controlled Analgesia (PCA) is such an extreme measure it requires multiple levels of authorization.
While the PCA was being organized, I was moved out of recovery to a private room on the delivery ward so I could receive one-on-one nursing care. Gena tried to help me transfer to a proper hospital bed, but I screamed with the pain of being moved and I hated the sensation of the catheter tapping against the inside of my bladder. I begged to stay on the recovery bed, so that’s what I slept on that night.
After getting settled in my new room, I was hooked up to the PCA pump. Gena threaded a tube under my nose. It looked like the kind that would deliver oxygen, but it had a little flap that covered my filtrum and bumped against my upper lip when I spoke. The flap measured my C02 output, because morphine can make you forget to breathe. If I stopped breathing, an alarm would be triggered. It was a clever device, but that little flap was really irritating.
The morphine kicked in, and I felt my body relax with exhausted relief that the pain had stopped. I had a moment of lucidity before sinking into a haze that I had a baby who needed to be fed. I began to worry that my milk wouldn’t come in, so asked DH to call my friend, E, who had generously offered me some of her pumped breast milk if I ran into problems and wanted to avoid formula-feeding V.
I wasn’t expecting to see them that evening, but E stopped by with her husband and their baby, bringing with them 100 ml of her breast milk and a giant bunch of pink and purple wildflowers. It’s hard to talk when you’re high on morphine – I remember being irritated at having to repeat myself multiple times, such was my slurring, and hating the feeling of the C02 monitor, like a heavy feather stuck to my lip – but I was overcome with gratitude. I think I said thank you and remarked on how big their baby had got, but I was otherwise a passive listener to the conversation.
Morphine is a strange drug. In that darkened windowless hospital room, every moment felt like it was 1am. It was like I was having an out-of-body experience – present but not really there – and it obliterated my memory except for the major discomforts.
The catheter sat uncomfortably in my bladder and against my leg. At the time, no one really understood what I meant, but the thick scab I had a few days later told me I’d been writhing in so much pain that the tube, just below where it was taped, had rubbed against my thigh and caused a deep blister. Even ten weeks on, I can see its faint scar, a slight darkening of skin.
But it was the itching that got me. It was like I’d swum in the ocean and let its saltwater dry on my back. Scratching only seemed to rub the ‘salt’ deeper into my pores. This confused me, but my night nurse appeared with a cool washcloth and wiped my back. She told me the next day that morphine makes you sweat and it’s excreted through your pores. In other words, morphine itches your skin. I craved those cool washcloths as much as I the water I begged to be allowed to drink. Later I was allowed sips of apple and orange juice in tiny cartons, but I gulped them down and asked for more. I also asked for food but was told I needed to wait until breakfast.
I was aware that V also needed to eat and that DH had to be the one to feed her. I wanted it to be me but gave in to the situation – namely, I was too high to hold her safely. As a newborn’s nutritional needs are so small she only needed a tiny amount of formula to supplement, so we chose not to use E’s breast milk. Her gift gave us options, which meant the pressure was taken off us. Besides, V had to be taught how to eat, which meant that temporarily using formula was more convenient. With his mom’s encouragement, DH cradled the baby in his left arm and held a syringe with 10 mls (two teaspoons) of formula in his left hand. His right hand was covered with a latex glove and he put a finger in V’s mouth. When she sucked, he delivered a little formula via a thin tube that was pushed inside her mouth. (This suck / reward system was a bit like training a dog!)
That night I kept awakening in pain, but the self-administered morphine was pretty quick to kick in. I’m not sure if you could say I slept – put into an artificially-induced drug coma would be more apt (hence the C02 monitor) – and DH barely closed his eyes. He confessed to constantly checking to see if V was still breathing, and even took her into the bathroom to prod her at one point. It was, for him, a stressful night after a long and harrowing day.
The Next Day
By daybreak, I was itching all over, had a parched mouth, and was ravenous. I agreed to be taken off the morphine as I needed to be transferred to the FMCC that morning. I had a final hit and was disconnected before being given oral meds that would help me transfer to my new hospital bed.
Even with morphine, moving from one bed to another was pretty ghastly. I raised my hips and inched my bottom to the edge of the bed. I grabbed the handrails for support and shifted my upper body over. Panting, I did it again to get right to the edge of the bed which was flush with my new bed. I didn’t care that my privates were on view. Right then, I had one goal, and that was to get to the new bed, dammit. It was the shortest marathon I never trained for.
There was no better gold medal for my efforts than to have V placed in my arms to breastfeed. I was given a silicone shield to help elongate my nipples and was transfixed by how this tiny, helpless red creature rooted and latched on. She sucked furiously and I could see that I was delivering colostrum. After nursing her, I pumped for the first time. Liquid gold. I suddenly understood why they call colostrum that. I pumped a total of 5 ml and my nurse was impressed. It was one of the proudest moments of my life to see that my body was able to produce food for my daughter.
Breakfast arrived and I devoured bland eggs, strangely scrambled into a pancake shape, and more tiny boxes of juice. Now that I was allowed to eat and drink, there was no stopping me – it had been 32 hours since I’d eaten anything. It wasn’t the best food of my life, but I was reminded of the bowl of cornflakes I’d enjoyed in October 1996. The cornflakes were stale and the milk powdered, but after sailing through a massive storm in the Indian Ocean, that bowl of cereal eaten perched on the rigging of a Chinese junk is the most memorable breakfast of my life. Cramming hospital eggs and a Dole fruit cocktail cup into my mouth after weathering a different kind of storm comes a close second.
After breakfast it was time to move to the post-partum ward. There wasn’t much to pack up. The little V burrito, swaddled and in a hat, was once again in my arms, the sides of the bed raised, and I left the delivery ward almost 36 hours after arriving.
I felt a bit like a celebrity, being wheeled to the elevators with this precious baby in my arms. I held her, at once fiercely protective and wanting to proudly show her off to every person we passed in the hallways. So this is what being a Mama Bear feels like.
A couple of floors up was the FMCC, where healthy babies room in with their mothers. I was disappointed to see that ours was a semi-private room – meaning I might have to share it with another family – but our day nurse, Emilie, said that she was going to try to keep it free for as long as she could. After everything you’ve been through, you deserve a nice big room, she said. True to her word, we had the room to ourselves for our entire stay, which meant DH got to sleep in a bed every night, instead of a reclining chair.
Once settled, the focus shifted to breastfeeding and healing. My MIL stayed with us, but my FIL excused himself because my breasts were constantly on display, nursing, pumping, or being looked at. There was a constant cycle of feeding: nursing supplemented with formula delivered via a syringe; pumping after nursing, making sure to get every last drop from the apparatus – even the drops from the bottle’s membranes were wiped off and onto my nipples to protect them; bottle feeding the precious colostrum; then MIL or DH would wash up everything, just in time for the cycle to start over again. In between feeds, I held V to my chest, skin to skin and we took photos.
Untethered, I got up for the first time half an hour after taking Percocet. I declined offers of help because others’ pulling felt too unpredictable for my battered body. Placing both hands behind one knee and then the other, I carefully bent my legs, raised my hips, and moved to the edge of the bed. I grabbed the handrail and pushed myself upright. Hands behind knees, I lowered my legs until I was sitting on the edge of the bed. I took a minute to catch my breath. I think I asked DH to hold my head to help me stand. My belly was on fire, and the area around my incision had a kind of tugging pain. When I was finally standing, I was bent double and had to lean on DH. Crossing the room to get to the bathroom took about a minute. It took another minute to pull down my mesh underwear and lower myself onto the loo seat. When I got back into bed, I was triumphant and exhausted. I knew the first time would be the worst time, and I had done it.
Healing and Learning
The post-partum ward marked the beginning of a never-ending stream of doctors, nurses, and med students whose rounds began at 5:30am. The worst part was most of them wanted to press my abdomen. At first even a gentle prod was enough to make me howl. After my SIL left, the pain returned with a vengeance. Emilie explained that the full effect of the spinal block and morphine had worn off. She was very good about bringing me my pain meds every four hours on the dot, but I think all the prodding after such a long surgery also caught up with me. Every time I got up to go to the bathroom was an exercise in pain management. My teeth chattered and my body shook with pain. I think what got me through these tough moments was having DH and MIL at my side, helped by having V in someone’s arms, if not my own, and safe the knowledge that the pain would pass, thanks to Percocet every four hours.
Dr. D stopped by for the first time since she went to get DH and V from the NICU. She said she couldn’t believe how well I looked for someone who had had “a pretty serious c-section” and was astonished to hear that breastfeeding, albeit with supplementation, was going well. She reiterated what others had said: that losing up to a litre of blood during a c-section is normal; that up to two litres was unusual; and 3.6 litres was utterly unheard of. I was pleased. I wanted her to know that I felt well looked after in her hands and her seeing me bounce back was proof of that. Dr. D explained that the reason for my blood loss was placenta accreta. She quoted me from the prenatal visit where I said, With my habit of falling into tiny statistics, if anyone is going to have any surprises on the day it’ll be me. The way she said it, it was like she was haunted by my premonition. The truth is, I had this feeling throughout my pregnancy that I had placenta accreta. I kept asking about it, complaining that my cervix didn’t feel right. Dr. D said, as she had done several times during my pregnancy, that my many ultrasounds had ruled it out, but my hunch proved correct. I was shocked, but not surprised.
During Dr. D’s visit, I heard DH recount his version of the events in the OR for the first time. I knew that it had been more traumatic for him in some ways – I may have looked terrible with my eyes rolling back in their sockets, but although it’s the closest I’ve ever come to death I never thought I would die that day. But DH couldn’t have known the conviction I felt. When he got to the part about being asked to leave the OR, his voice broke and he began to cry. Unable to reach over to him, I watched his face crumple as he apologised for the pause. Dr. D put her hand on his shoulder and reminded him of what she had said at our prenatal visit – that in some ways, being the support person in the OR is far more traumatic. She shared that her husband had been freaked out when their first daughter was born. Something about her birth required that she stay in the NICU overnight and she had a tube going into her scalp which her husband found very upsetting. I am very lucky that my OB is so compassionate, as well as skilled.
Dr. C, V’s paediatrician, also stopped by on her way home from church. I was especially touched by this, because it meant that she had made a special trip in to check on us. Dr. C told us when we first met her that this was something she liked to do, but I began to get the impression that the story of V’s birth was making the rounds. You lost 3600 ml and you seem to be recovering extremely well. And how amazing that you are breastfeeding! I found this consistent praise quite empowering. My genes may have failed me, but my body hadn’t.
It seemed that the next comment was always about V’s hair. A common refrain was Look at her hair! so I looked at her hair. It was red. Or was it strawberry blonde? It was a bit like the colour of earwax – orangey and golden. I’d always pictured my kiddo having dark hair. At first I was taken aback by the red, so unlike anything I’d seen in my genetic family. I thought of a story a schoolfriend, A, shared about her birth – her dad sighed, “Oh no, she has red hair…” Perhaps his was too? I wasn’t sure why anyone would have been disappointed to see A’s lovely red curls. I looked at my daughter’s little mop of messy hair and, foreign though it may have been to me, thought it was extremely pretty. But as Emilie showed us how to hold V and wash her hair under the faucet, I asked why everyone kept commenting on it. Emilie explained that most fair-haired babies are born with very sparse hair, if they have any at all. Usually only dark-haired babies have full heads of hair. This made sense to me. Thinking of the babies I know, all the blonde ones are totally bald.
Sunday also marked laughing for the first time. As I painfully made my way across the room, hunched over like Quasimodo, my FIL said Girl, you’re all set for Halloween! It was October 26th, so I wanted to roar with laughter, but had to avoid roaring in pain instead. I panted my laughter from the top of my chest, great heaving exhalations between gasps of Please don’t make me laugh!
That evening, I took my first post-partum shower. My night nurse, Dilliam, a plump grandmotherly woman from Panama, got everything set up for me. She was delighted that I speak Spanish but assured me, in her thick-accented English, that she would “loog after de lickle baby” while MIL helped me shower. I’ve always had cool showers, but that evening I turned up the water so hot I could barely stand still under it. It felt so good I almost cried. (The strange thing is, I’ve enjoyed my showers like this ever since.) Renewed, I even took a stroll around the corridors, pushing V in her bassinet for support.
I trusted Dilliam to take V for a couple of hours that night so DH and I could get some sleep. When she was returned to me, she smelt like Dilliam’s perfume and knew she’d been cuddled. I mentioned this to Emilie who grinned and said, Did you hear Dilliam washed V’s hair again? Even though Emilie had shampooed V less than 12 hours earlier, Dilliam washed it a second time because “she didn’t believe it was really that colour.” DH and I still chuckle about this.
Monday was when I began feeling like myself again. I’d thought that pregnancy had pushed my body to its limit, but recovering from losing a gallon of blood during a three-hour-long caesarean tested me in other ways. Yet, if I had been physically able to, I’d have been bouncing off the walls in spite of the sleep deprivation. To my astonishment, it was DH – not me – who was struggling with the lack of sleep. Usually he gets by fine on a few hours’ sleep, but I think the PTSD was getting to him, so Sunday and Monday afternoons he returned home for a long nap, leaving me with MIL for company. I didn’t mind at all. Go! I reassured him. You’ll be much more useful to me if you are rested. Somehow I was making it through the day, no doubt helped by the coffee I was enjoying for the first time in almost 18 months. But I felt – and still feel, writing this ten weeks later – that something biological was afoot. There is no other explanation for how I am surviving on so little sleep, what I affectionately have called a ‘sustained fuck all’.
Monday was also the day I met with a third lactation consultant, Carole. Perhaps it was because I was producing colostrum reliably at this point, but I feel it was Carole who really put me on the path to exclusively breastfeeding. She showed me how to massage the hard knots of milk out of my breasts, and it was she who devised the feeding schedule: nurse with supplement formula in a syringe every three hours, then bottle-feed whatever I was able to pump from the end of the previous nursing session. Nursing and pumping regularly would help establish my milk supply. How those first pumping sessions hurt! I couldn’t believe that my IRL IF friend was able to crank up the pump all the way…
A few hours before we were discharged, Carole weighed V before, during, and after a feed, to calculate how much colostrum I was producing. To her amazement, V had eaten 37 ml (1¼ oz) in one feeding session – an amount which twice appears in my medical records with a exclamation mark! I cocked my head and asked if I needed to supplement with as much formula. Carole’s response was to tear up the notecard with my former breastfeeding instructions. Somehow, in spite of a history of IVF, being over 35, and, most critically, losing a massive amount of blood, I was exclusively breastfeeding on the day of discharge!
Going Home
I dressed V for the first time: a white onesie with a blue cherry print. After we raided the hospital room for spare packs of diapers and wipes, DH made multiple trips to the car. He returned with V’s car seat which California requires by law parents to provide. Without it, the hospital cannot release a baby. Lindsay, our discharge nurse, showed us how to tighten the harness so it was snug enough so you can’t pinch the belt, but not so tight that you can’t slide two fingers underneath. V was dwarfed by the car seat and screamed the mewling kitten cry of a miserable newborn. Lindsay picked up the car seat and, pivoting it against her body, swung it from side to side to soothe the baby.
My discharge paperwork was produced quickly, but V’s took a while. Her heart murmur – common in young newborns – had disappeared, but she was still a little jaundiced. The post-birth weight she’d lost so drastically (11%) at first had tapered off, leaving the paediatric nurse practitioner to believe her birth weight of 7 lbs 11 oz had been artificially high due to the fluids I received in my IV. It certainly explained why her features were so swollen at birth. We were scheduled to follow up with Dr. C a few days later. V’s jaundice disappeared without the need for light therapy, and she began gaining weight at a rate of 50 g a day at one point (paediatricians like to see a minimum of 25 g, so this was very good).
Post-Partum Conclusions
At my first post-partum checkup ten days after delivery, I thanked Dr. D for getting both V and me out the OR safely. She replied that she was glad she was there, that it was not something she would have wanted to hear about from someone else. Again, I am reminded of how important it is to have a doctor whom you like and trust, and who likes and respects you as a patient.
At my second, six-week post-partum visit, Dr. D explained that the pathology report on my placenta diagnosed villitis, which can cause IUGR, so if we want a second baby it will be a high-risk pregnancy with frequent ultrasounds to make sure the baby is growing well. Apart from that, I have a clean bill of health.
Dr. Google says villitis is also associated with stillbirth. It’s too early to think about seriously, but between the risks of stillbirth and hysterectomy, I may not have the second child I’d always assumed I’d have. My loss and infertility journey has taught me that things don’t always work out the way you want them to. V is enough. If we can’t give her a brother or sister – which I’d like to for all sorts of reasons, including having someone she can discuss her genetic origins with – I trust we’ll muddle through, the way we seem to. (This muddling through is another blog post in and of itself.)
I wished Dr. D happy holidays but it wasn’t until after she’d left the room that I realized it’s going to be a while until I see her again – although she is my gynaecologist as well as my obstetrician, I’m not due for a pap smear for another year or so. In fact, it’s the first time in over a year that I’m not seeing a doctor or nurse on a very regular basis. It felt strange to be released from my RE, and stranger still to be released from my OB. All this time spent getting and staying pregnant, the dozens of ultrasounds, injections, blood draws, the thousands of miles driven to and from appointments, the money, the soul-searching – has made me a better parent. Which is not to imply that loss and infertility are a pre-requisite to good parenting, or that I would have been a shitty parent without it. All I can say is that my experience has made me stronger.
Sweet V
I look at my daughter today – 10 weeks and 2 days old, sucking ferociously, a person who can anticipate being fed and having her diaper changed, a regular social smiler, and someone who is beginning to laugh – and know she, too, is strong. Not just because of her swift weight gain. Not just because of her determination to hold up her head. Not just because of the kicks I miss feeling from the inside. I’ve known from those two pink lines that she is a fighter: because of the 28 eggs we inseminated, 21 fertilised; and of the 21 embryos, there were always two that were always slightly ahead of the rest. By the day of transfer, our embryos had survived six days in a petrie dish and had been biopsied for genetic testing. But it was Embryos 3 and 4 – euploid male and female, respectively – who were fully hatched and raring to go. And Embryo 3 – aka Baby B or ‘Indigo’ – didn’t quite make it, but his sister, Embryo 4, clung on for dear life.
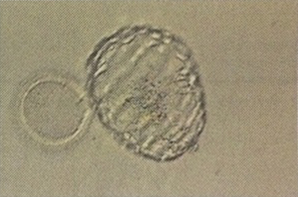
Feb. 26th 2014: V as six-day-old fully hatched blastocyst
V is here and, as she has done from the moment of her conception, she is thriving.

Thank you for documenting all that. It was a fantastic roller coaster of a ride. V is beautiful.
It was a roller coaster to live it, lemme tell you! Thank you! She is the apple of my eye <3
Beautiful!! So happy for you all xxx
Wow Lauren. You went through so much to have V here safely. She is gorgeous!
I sure did! Thank you for acknowledging that. But you know what? I’d do it all over again…
Btw, you were the second most frequent commenter on my blog last year! Thanks! Xoxo
Wow. I don’t have time at the moment to read the whole story, so will have to come back. Just wanted to comment on how amazing your photos are, however. In the second photo you look like a Madonna painting. :-) So glad to hear things are going well with V.
Blimey, that’s a hell of a compliment! Take your time! I know how it goes… Xoxo
Thank you for sharing. A great read. Emotional closure.
Phewf! What an emotional roller coaster, and that’s just reading about it! You truly are an amazing woman, with an amazing DH and bubba too!
Wow, this was SO amazing to read. What a blessing to have it all documented for you to read back on. It’s fairly amazing to me how quickly the details fade from our birth experiences, even when that seems impossible in the immediate aftermath. Thank you so much for sharing your story!
Thank YOU for reading! It was really important to me to write it, and almost as important to be able to share it with others x